How to Manage Labor Pain Like a Boss: All Your Options, Explained
“Gimme the drugs!”
You hear that line screamed a lot in movies and TV shows from sweaty laboring women, and we all know what it means: Give me an epidural!
But what exactly is an epidural, and what does it mean for your birth journey? What other pain management options are out there? And how to decide what the best options are for YOU?
Let’s break it down so you can have the info you need to rock your labor like the boss you are :)
Epidurals
Over 50% of people giving birth in the US get either an epidural or spinal block during labor. The main perceived benefit is that they’re considered the most effective form of pain relief, especially when compared to medications given intravenously. As you make your birth plan and prepare for babe’s arrival, it’s important to understand the benefits and risks of this type of pain management so you can make informed choices about your options before and during labor...so here’s the scoop!
The Big 3
Epidural Block
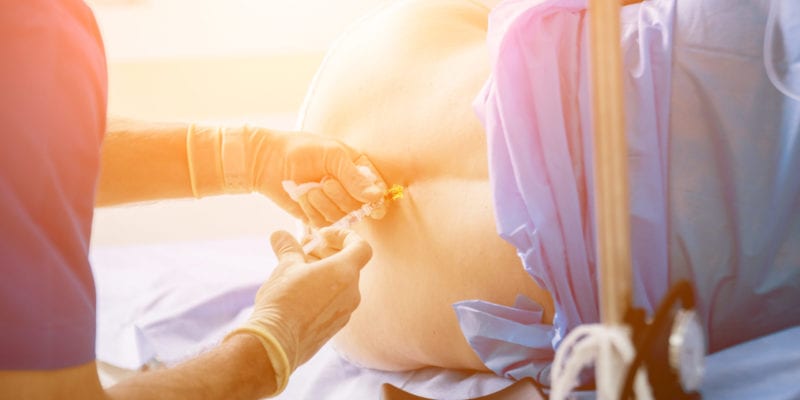
Your spinal cord and nerves are contained in a sac of cerebrospinal fluid, and the space around this sac is called the epidural space. When you receive an epidural, numbing medications (usually a combo of narcotics and anesthesia) are injected into that surrounding space...hence the name! Epidurals are used for either vaginal births or cesareans, since the dosage level can be adjusted higher or lower to provide a complete absence of sensation (total anesthesia) or a light pain relief effect (analgesia). Ideally, with a light epidural, your pain level decreases but you can still move your legs and push your baby out on your own.
The doc or nurse will place a catheter into the epidural space using a guide needle, and then the catheter is taped in place so that the meds can be administered as needed. A light epidural (i.e. less anesthetic) should allow you to be more active in your labor, although you will likely be required to remain lying down in bed for the duration. Each hospital will have different policies re: staying in bed, eating and drinking with an epidural, so check with your provider.
After delivery, the catheter may come out immediately or it may be left in for up to a day (this is more common after a belly birth, so you can keep receiving pain meds as needed).
Spinal Block
A similar procedure to an epidural, but the numbing medication is injected directly into the spinal fluid sac. Because of that, the effect is more immediate, so these are used more commonly in emergency situations or for scheduled cesarean births when mama is not already in labor. The medication is given in a smaller dose so it usually only lasts an hour or two.
Combined Spinal - Epidural Block (CSE)
Basically exactly what it sounds like...you’ll get the injection into the spinal sac for immediate anesthetic effect, and then a catheter will be inserted into the epidural space to maintain the effect.
Why Might You Want One?
There are a few reasons you might opt for an epidural:
- General pain relief / pain management in labor
- A belly birth
- To provide rest to mama during a long or exhausting labor
The success of an epidural depends a lot on the skill with which it’s administered; techniques and medication combinations are constantly being refined and different providers will have different options for you.
Things To Know
Anytime you opt for an intervention in the physiologic birth process you are medicalizing your birth at least a little bit, and epidurals are no exception…here’s what you might experience along with the analgesic effect:
- Continuous monitoring of both your vitals and baby’s → this means being hooked up to monitors that will check stats like blood pressure and oxygen levels, and fetal and contraction monitors around your belly, which may restrict your movement
- An IV drip delivering extra fluids and possibly Pitocin to augment or speed up your labor
- A catheter in your bladder since you won’t be able to feel the need to pee
Common risks of epidurals can include things like:
- Heavy motor-blockade → your legs might become so heavy and hard to move that you cannot move the lower part of your body at all
- Fever during labor
- Itchy skin
- Higher likelihood of needing forcep or vacuum assistance with delivery
- Hypotension (fancy word for low blood pressure)
- Longer first and second stages of labor due to the epidural slowing your labor progress; this might mean augmentation with Pitocin (a synthetic form of oxytocin)
- Medications used in your epidural do cross the placental barrier, which means they could have a temporary effect on your baby. Research is ambiguous as to whether this can directly lead to nursing challenges post-birth; check out Evidence-Based Birth for a breakdown of the available info
- Increased risk of unplanned cesarean → this depends a LOT on your care provider, since it’s especially important for docs to follow best practices when it comes to epidurals to help prevent unnecessary belly births
Less common risks of epidurals include:
- Inadequate pain relief; epidurals don’t work for about 10 - 12% people who receive one
- Spinal headache from leaking spinal fluid
- Slowed breathing or drowsiness in mama
- Infection at the injection site
- In very rare cases, permanent nerve damage, seizures, and severe breathing difficulty have occurred.
In some cases an epidural isn’t a viable option at all; if you have certain health conditions or are on certain medications, if you are not at least 4 cm dilated, if your doc cannot locate the epidural space to place the catheter, or if your labor is moving too quickly to get the meds going.
Mama Pro Tip → Epidurals can be a part of something called the “cascade of interventions,” which basically means that once you get one intervention in labor you may be more likely to receive subsequent ones, up to and including an unplanned C-section. As part of your birth prep, we recommend bringing up any concerns or questions you have about this to your care provider so you can feel prepared and advocate for your wishes!
Non-Medical Pain Management
If you’d prefer to skip the epidural, or are unable to receive one for some reason, there are a variety of non-medical options for pain management during labor. Check out our list below, and as always please do your own research and ask your provider as many questions as you want!
-Miles Circuit-Spinning Babies
-counterpressure
-Rebozo sifting
-Hypnobabies
-breathwork
-mantras/affirmations
-hydrotherapy via shower or bathtub
-massage
-changing positions / staying mobile
-using a birth ball or peanut ball
-mindfulness exercises / expectation
-nitrous oxide (this one is a more medical option, but it’s considered extremely low risk and since you control your use of it, you decide how much or little you need throughout labor)
All of these methods carry little to no risk to you and baby, and can be used in combination with each other to maximize their efficacy.
Mama Pro Tip → Regardless of whether you want an epidural, plan to have a belly birth, or are hoping to birth without interventions or medications…HIRE A DOULA!! You deserve as many people in your corner as possible when mapping out your desires for your childbirth experience, and a doula can help you advocate for yourself in the birth space, is 100% there for you (and your partner if you have one), and comes with tools and experience for managing labor pain and assisting you in post-birth recovery. Can’t say it enough…doulas are golden.
Bottom line? There are many options available to you for effective pain relief during labor and birth, and the most important thing is that you feel empowered and informed to make the choices that are best for you. It also should go without saying that ALL births are incredible and ALL birthing people are incredible...no matter how the heck that baby comes out! Whatever you decide and whatever happens, you are an amazing mama :)
***************
As always, remember that while all of us at AMMA are brilliant and passionate about all things motherhood, none of us are medical professionals! Always speak with your care provider to get the go-ahead on anything concerning yours or baby’s well-being.